Medically Reviewed by KLE Doctor
Written by KIE Editorial Contributors
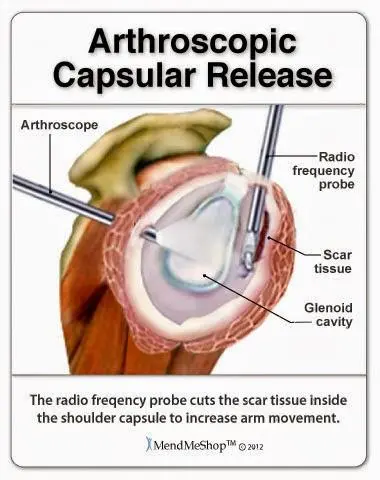

Frozen shoulder, or adhesive capsulitis
, is a term that describes a condition in your joint that starts out with pain, then progresses into stiffness and lack of mobility, then eventually returns to normal. It generally strikes adults between the ages of 40 and 60, and tends to affect women more than men. On visualizing the joint with scope we would find thickened ligaments and cartilage, swelling, and excessively tight connections — maybe even some scar tissue
Although an injury can lead to a frozen shoulder, it’s generally not the cause of it. long stints of immobility cause the tissues in your shoulder to swell, thicken, and stiffen. Likewise, extended illness or even surgery — anything that makes you sedentary — can contribute to frozen shoulder syndrome. Diabetes and thyroid conditions also put you at greater risk for frozen shoulder, so properly monitoring your symptoms can help you prevent your shoulder from seizing up.
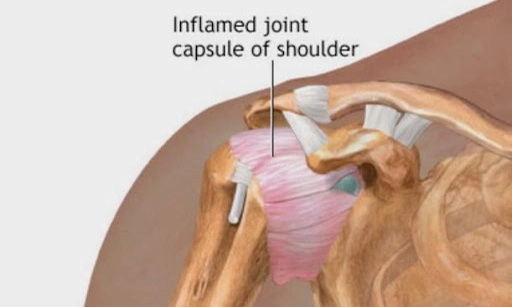
Stages of frozen shoulder -
Typically, frozen shoulder progresses through three stages of development over a period of about two or three years.
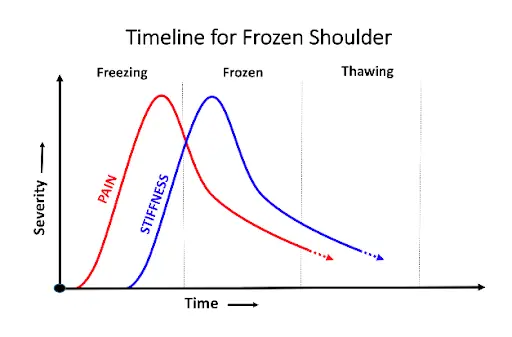
Given enough time, your frozen shoulder may resolve itself without intervention, but three years is a long time to go without the use of your shoulder. Here are your treatment options.
Although it may seem counterintuitive (and painful), movement is the best medicine for your frozen shoulder. There is no substitute for physical therapy, including passive stretches and strategic flexes that encourage your joint to speed up the healing process. It may help to apply gentle heat to your shoulder before your exercises and ice afterward.
Since inflammation is one of the main culprits causing your frozen shoulder, reducing that swelling can bring you significant pain relief. Over-the-counter anti-inflammatory drugs (NSAIDs) such as ibuprofen and aspirin can take the edge off your intense pain so that you can continue with your physical therapy.
Surgery is not always necessary to treat adhesive capsulitis, but when scar tissue has built up and your body won’t heal itself, you may need to have some of that extra tissue removed. There are two main ways we can help.

Both have excellent outcomes depending on what stage the presentation is, but in most cases full recovery is expected. Hence early diagnosis and physical therapy is imperative.
Dr. Nikhil Manvi Assistant Professor MBBS, MS Orthopedics, Fellowship in Joint replacement and Fellowship in Arthroscopy.
Get in Touch with a Doctor